Fallstudien

Vorgestellte Fallstudie
So steigerte Maxion Wheels die Einsparungen durch kontinuierliche Verbesserung dank Minitab Engage um 19 %
Maxion Wheels, der weltweit größte Hersteller von Autofelgen, steigerte die jährlichen Kosteneinsparungen um mehr als 19 %, indem das Unternehmen Minitab Engage® in sein Projektmanagementsystem aufnahm. Die Engage-Infrastruktur ermöglichte eine unmittelbare Transparenz und verständliche Kennzahlen in 1.600 Projekten mit 1.500 Benutzern, was zu einer verbesserten Produktivität und Zusammenarbeit führte.

Vorgestellte Fallstudie
So konnte die USC Consulting Group einen führenden Süßwarenhersteller dabei unterstützen, mit der Minitab Statistical Software Überfüllungen zu reduzieren und 1,2 Millionen Dollar einzusparen
Seit über 50 Jahren setzt sich die USC Consulting Group (USCCG) für Operational Excellence ein. Ihre Mission ist dabei, echten Mehrwert durch eine Optimierung der Finanzperformance zu schaffen. Die USCCG unterstützt Unternehmen dabei, ihr Potenzial zu realisieren, indem Prozesse und Abläufe in der gesamten Lieferkette verbessert werden.

Vorgestellte Fallstudie
Qualität in allen Farben: Wie Crayola Daten zur Produktion des perfekten Wachsmalstifts nutzt
Die Datenanalyse und Umsetzung der Ergebnisse hat bei Crayola die Abläufe verändert und das Unternehmen in die Lage versetzt, Ressourcen da zu konzentrieren, wo sie am effizientesten eingesetzt werden können.

Vorgestellte Fallstudie
So lässt Tate & Lyle Süßstoffe mehr wie Kristallzucker wirken
Als bei der Raffinade von Dextrose Probleme auftraten, zog Tate & Lyle die Minitab-Software heran.
Vorgestellte Fallstudie
Der perfekte Einstieg in die Statistik für Trainees: Cummins vertraut auf den Quality Trainer
Durch den unterschiedlichen Kenntnisstand der Mitarbeiter bei Cummins Inc. in Bezug auf Statistik stellte die Schulung von Six Sigma-Trainees eine Herausforderung dar. Daher setzte das Unternehmen den Quality Trainer by Minitab ein.
- Automobilindustrie
- Energie und Ressourcen
- Finanzen
- Behörden
- Gesundheitswesen
- Fertigung
- Medizintechnik
- Bergbau
- Qualitätsverbesserung
- Dienstleistungen

Bobcat
Ein Qualitätsexperte bei Bobcat steigerte mithilfe der Minitab Statistical Software die Geschwindigkeit eines Laserschneidevorgangs bei gleichzeitiger Verbesserung der Teilequalität, was zu möglichen Einsparungen von über 1 Million US$ führte.
.png)
DOE bei der Ford Motor Company
In Anbetracht der anstehenden Markteinführung des Ford Fiesta verließ sich die Ford Motor Company auf Minitab, das die erforderlichen Werkzeuge bot, um ein hochwertiges Produkt und einen erfolgreichen Produktstart zu ermöglichen.

Maxion Wheels
Maxion Wheels, der weltweit größte Hersteller von Autofelgen, benötigte unmittelbare Transparenz in Bezug auf seine Projekte für die kontinuierliche Verbesserung und Operational Excellence. Das Unternehmen entschied sich für Minitab Engage. Diese Lösung bot Workflow-Funktionen, mit denen die Stakeholder den Fortschritt ganz einfach auf der Grundlage von Daten, die sichtbar für die Administratoren sind, nachverfolgen und berichten können. Dadurch konnte das Unternehmen die Transparenz verbessern sowie Zeit und Kosten sparen.
Globaler Anbieter von Solartechnologie und erneuerbarer Energie
Eines der größten Unternehmen im Bereich Solartechnologie und erneuerbare Energie musste die Stärke der Siliziumnitridschicht unter Kontrolle bringen, um die Energieeffizienz zu verbessern. Erfahren Sie, wie das Unternehmen die Ursachen für die Unterschiede bei der Schichtstärke mit den leistungsstarken Diagramm- und Analysewerkzeugen in der Minitab® Statistical Software und in Minitab Engage® ermitteln und beheben konnte.

Fresnillo Plc
Fresnillo Plc steigerte den monatlichen Umsatz um über 2 Millionen US-Dollar, indem mit Lean Six Sigma-Methoden und der Minitab Statistical Software der Silbergewinnungsprozess in der Saucito-Mine untersucht wurde.
.png)
Mosaic Corporation
Erfahren Sie, wie ein Six Sigma-Team der Mosaic Corporation mit seinen umfassenden Erfahrungen bei der Prozessverbesserung und mit leistungsstarken Werkzeugen wie der Minitab Statistical Software die Produktivität um mehr als 50 Prozent steigern konnte, was 12 Millionen US$ pro Jahr entspricht.

Newcrest Mining Ltd
Durch die Minitab Statistical Software kann Newcrest Mining in der Cadia Hill-Mine mit jedem LKW eine zusätzliche Ladung Erz pro Tag befördern.

Grupo Mutual
Ein Projektteam bei der Grupo Mutual, eines der führenden Finanzinstitute Costa Ricas, wollte den Cashflow zwischen 55 ihrer Bankfilialen verbessern. Mit Lean Six Sigma-Methoden und der Minitab Statistical Software konnte das Team die Erträge um 1,1 Millionen $ steigern.

Edward Jones
In Anbetracht des derzeitigen Wachstums des Finanzdienstleisters und seiner Expansionspläne wollte Edward Jones sicherstellen, dass der erstklassige Kundendienst auch künftig die Erwartungen der Kunden übertrifft. Ausgerüstet mit Lean Six Sigma-Strategien und den Statistikwerkzeugen in der Minitab Statistical Software begann das Prozessverbesserungsteam bei Edward Jones zu untersuchen, wie das Unternehmen bei ständig steigenden Anforderungen weiterhin die hohen Standards beim Kundendienst einhalten konnte.

Tyler, Texas
Die Stadt Tyler in Texas konnte mit Lean Six Sigma-Projekten mehr als 5 Millionen US$ einsparen. In einem dieser Projekte wiesen Mitarbeiter der Stadt mit Hilfe der Minitab Statistical Software nach, dass sich mit einer geringeren Menge Magnesiumhydroxid immer noch die bundesstaatlichen Vorschriften erfüllen und dabei ca. 80.000 US$ an Kosten einsparen ließen.

City of Fort Wayne, Indiana
Durch Minitab konnte die zweitgrößte Stadt in Indiana ihre kommunalen Leistungen optimieren – und Millionen von Dollar sparen.

Takeda steigert Medikamentenproduktion mit Hilfe von Modellen für maschinelles Lernen
Als die Takeda Pharmaceutical Company Ltd. effizienter größere Mengen seiner drei Blutgerinnungspräparate produzieren wollte, setzte das Unternehmen die Funktionen für maschinelles Lernen der Minitab Statistical Software ein, um eine Möglichkeit zum Steigern der Ausbeute aus den in der Produktion eingesetzten Zellkulturen zu ermitteln.

Lehigh Valley Health Network
Das Lehigh Valley Health Network (LVHN) hat in seiner über hundertjährigen Geschichte bereits einige wichtige Qualitätsziele erreicht. Vor Kurzem kamen Lean Six Sigma-Werkzeuge und die Minitab-Software für statistische Analysen zum Einsatz, um Verbesserungen bei der Versorgung der Patienten zu ermöglichen.

Connections Health Solutions
Aufgrund von Problemen im Qualitäts- und Sicherheitsbereich wurde Connections Health Solutions im April 2014 beauftragt, die Leitung des Crisis Response Center in Tucson, Arizona, zu übernehmen. Connections verfügte bereits über langjährige Erfahrungen mit dem Betrieb eines solchen Notfallzentrums in Phoenix und strukturierte die Prozesse für die Evaluation, Aufnahme und Behandlung von Patienten mit Lean Six Sigma-Methoden neu. Mit der Minitab Statistical Software konnte das Team von Connections seinen Erfolg messen. Hierzu gehörten erhebliche Verbesserungen beim Zeitmanagement, der Qualität der Versorgung und der allgemeinen Patientenzufriedenheit.

Riverview Hospital Association
Mit der Minitab Statistical Software konnte das Lean Six Sigma-Team der Riverview Hospital Association Daten analysieren, um Patientengruppen zu identifizieren, die bei Umfragen zur Patientenzufriedenheit niedrigere Werte erzielten. So konnte das Team Prozessverbesserungsinitiativen gezielt auf bestimmte Patientengruppen ausrichten.

RightSource
Als die Apotheke RightSource ein neues Rezeptverwaltungssystem einführte, sank die Produktivität, und Bestellungen fielen in den Rückstand. Durch Umsetzung eines Lean Six Sigma-Projekts mit Minitab konnte das Unternehmen den Umlaufbestand um 40 % reduzieren und bei jedem Arbeitsschritt Geld sparen.

Cathay General Hospital
Bei einer Auswertung des Angioplastieverfahrens für Herzinfarktpatienten analysierte das Cathay General Hospital in Taipeh (Taiwan) mit der Minitab Statistical Software Daten, um Leben zu retten. Mit den von Minitab bereitgestellten Werkzeugen konnten Medizinexperten neue Behandlungsoptionen einführen, die zu einer Verkürzung des Krankenhausaufenthalts für die Patienten und höheren Einsparungen bei medizinischen Ressourcen führten.

Hauspflege durch das Akron Children’s Hospital
Das Akron Children’s Hospital untersuchte den Abrechnungsprozess für die Hauspflege mit Lean Six Sigma-Methoden und der Minitab Statistical Software. Die Datenanalyse führte dazu, dass sowohl zu Hause als auch ambulant behandelte Patienten eine optimale medizinische Versorgung erhalten und die Anzahl der Tage zwischen der Produktauslieferung und der Rechnungsstellung um 90 % reduziert wurde.

Boston Scientific
Bei der jährlichen Bewertung seiner Materialien und Prozesse verwendete der Medizingerätehersteller Boston Scientific die Minitab Statistical Software zum Analysieren von Daten für die Überprüfung des Prozesses, mit dem die Beutel zum Verpacken der Führungsdrähte versiegelt werden. Mit den Werkzeugen in Minitab konnten die Ingenieure souverän mit der Verwendung eines neuen Beutels beginnen, durch den die Verpackung in verschiedenen Unternehmensbereichen optimiert und wesentliche Einsparungen bei den Materialkosten erzielt wurden.

Via Christi Health
Mit der Einführung des Center for Clinical Excellence bei Via Christi stellte der Gesundheitsdienstleister ein Team von 5 Mitarbeitern zusammen, die alle Lean- und Six Sigma-Schulungen absolviert hatten. Diese entwickelten Projekte, mit denen die Versorgung der Patienten einheitlicher und die Effizienz der Abläufe gesteigert werden sollten. Für die Datenanalyse, die für die verschiedenen Projekte benötigt wurde, verließen sich die Prozessverbesserungsteams von Via Christi auf die Minitab Statistical Software.

Extubationen am Akron Children’s Hospital Center
Der größte Anbieter im Bereich Kindermedizin im Nordosten Ohios analysierte mit Minitab die Daten eines Lean Six Sigma-Projekts. Dies führte zu einer Reduzierung der Anzahl ungeplanter Entfernungen von Beatmungsschläuchen bei Kindern auf der Neugeborenen-Intensivstation und damit zu weniger Komplikationen und einer Verkürzung der Aufenthaltsdauer.

Akron Children’s Hospital
Der größte Gesundheitsdienstleister im Nordosten Ohios setzt Qualitätsverfahren aus der Industrie ein, um die Wartezeiten der Patienten zu verkürzen und eine Vielzahl weiterer Verbesserungen einzuführen. Zum Analysieren der Daten und zum Interpretieren der Ergebnisse verlassen sie sich auf die Minitab Statistical Software.

KYOCERA AVX verleiht der Kundenstimme Priorität
KYOCERA AVX nutzte Minitab Engage, um Einblicke in seine Qualitätsmanagementsysteme und Programme für die kontinuierliche Verbesserung in den Werken weltweit zu erhalten. Durch diese Initiative wurde die Zusammenarbeit verbessert, es gab neue Lernchancen, und die Kunden wurden schneller und effizienter betreut.

Takeda steigert Medikamentenproduktion mit Hilfe von Modellen für maschinelles Lernen
Als die Takeda Pharmaceutical Company Ltd. effizienter größere Mengen seiner drei Blutgerinnungspräparate produzieren wollte, setzte das Unternehmen die Funktionen für maschinelles Lernen der Minitab Statistical Software ein, um eine Möglichkeit zum Steigern der Ausbeute aus den in der Produktion eingesetzten Zellkulturen zu ermitteln.

USC Consulting Group
Seit über 50 Jahren setzt sich die USC Consulting Group (USCCG) für Operational Excellence ein. Ihre Mission ist dabei, echten Mehrwert durch eine Optimierung der Finanzperformance zu schaffen. Die USCCG unterstützt Unternehmen dabei, ihr Potenzial zu realisieren, indem Prozesse und Abläufe in der gesamten Lieferkette verbessert werden.

Hexpol
Die Experten bei HEXPOL Compounding, weltweit führend bei der Herstellung von Gummimischungen, sind stolz auf ihre Marktkenntnisse und Innovationskraft, durch die sie Kunden in verschiedenen Branchen – von Automotive, Bauwesen und Gesundheitswesen bis hin zu Energieversorgern und der Öl- und Gasgewinnung – die richtigen Lösungen für ihre Anwendungen bereitstellen können.
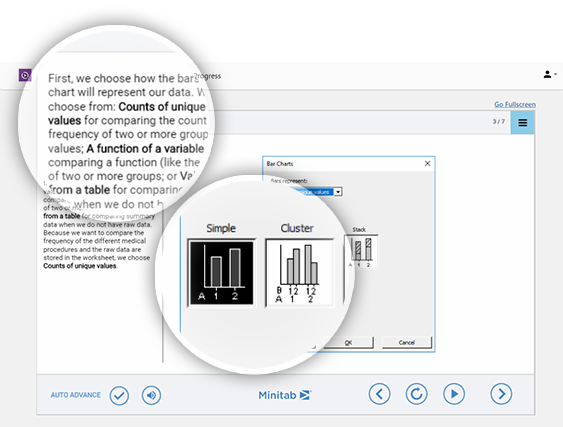
Tate & Lyle
Tate & Lyle ist ein führender Hersteller im Lebensmittelsektor und hat eine lange und erfolgreiche Geschichte. Gemäß seinem Slogan „Making Food Extraordinary“ produziert das Unternehmen aus Mais, Tapioka und anderen Rohstoffen Zutaten, die Nahrungsmitteln Geschmack, Textur und Nährstoffe verleihen. Eines der bekanntesten Produkte in den USA ist der Süßstoff SPLENDA® (Sucralose). Als bei der Raffinade von Dextrose Probleme auftraten, zog Tate & Lyle die Minitab-Software heran.

Crayola
Die Datenanalyse und Umsetzung der Ergebnisse hat bei Crayola die Abläufe verändert und das Unternehmen in die Lage versetzt, Ressourcen da zu konzentrieren, wo sie am effizientesten eingesetzt werden können.

Anheuser-Busch InBev
Anheuser-Busch InBev reduzierte die Ausfallzeiten in der Produktion für den Wechsel zwischen verschiedenen Biermarken um 34 % und konnte über 430.000 US-Dollar einsparen.

Thai Roong Ruang Sugar Group
Die Thai Roong Ruang Sugar Group, der führende Zuckerexporteur Thailands, setzte die Minitab Statistical Software ein, um den Prozess bei ihren Mitarbeitergesprächen auszuwerten und zu standardisieren und damit einer potenziellen Voreingenommenheit bei den Managern vorzubeugen. Durch eine Analyse der Daten konnte das Team ein faires Vergütungsschema aufstellen, bei dem unfaire Beförderungen vermieden werden.

Boston Scientific
Bei der jährlichen Bewertung seiner Materialien und Prozesse verwendete der Medizingerätehersteller Boston Scientific die Minitab Statistical Software zum Analysieren von Daten für die Überprüfung des Prozesses, mit dem die Beutel zum Verpacken der Führungsdrähte versiegelt werden. Mit den Werkzeugen in Minitab konnten die Ingenieure souverän mit der Verwendung eines neuen Beutels beginnen, durch den die Verpackung in verschiedenen Unternehmensbereichen optimiert und wesentliche Einsparungen bei den Materialkosten erzielt wurden.

Medtronic
Die Black Belt-Kandidaten bei Medtronic haben unterschiedliche Kenntnisniveaus bei ihrer Vorbildung, was Schulungen erschwert. Um sicherzustellen, dass die Kandidaten in Bezug auf die statistischen Methoden auf dem gleichen Stand sind, und um deren Erfolgspotenzial zu maximieren, entschied sich Medtronic für den Quality Trainer, den E-Learning-Kurs von Minitab für Statistik für die Qualitätsverbesserung.
.png)
DOE bei der Ford Motor Company
In Anbetracht der anstehenden Markteinführung des Ford Fiesta verließ sich die Ford Motor Company auf Minitab, das die erforderlichen Werkzeuge bot, um ein hochwertiges Produkt und einen erfolgreichen Produktstart zu ermöglichen.

Cummins
Durch den unterschiedlichen Kenntnisstand der Mitarbeiter bei Cummins Inc. in Bezug auf Statistik stellte die Schulung von Six Sigma-Trainees eine Herausforderung dar. Daraufhin probierte das Unternehmen den Quality Trainer by Minitab aus, einen E-Learning-Kurs, in dem Green Belts, Black Belts und andere Qualitätsexperten die Statistikkenntnisse erwerben können, die sie benötigen. Durch die Integration des Quality Trainers in das Schulungsprogramm konnte Cummins mehr Mitarbeiter in Six Sigma-Projekte einbeziehen.

Bobcat
Ein Qualitätsexperte bei Bobcat steigerte mithilfe der Minitab Statistical Software die Geschwindigkeit eines Laserschneidevorgangs bei gleichzeitiger Verbesserung der Teilequalität, was zu möglichen Einsparungen von über 1 Million US$ führte.
Stryker
Stryker, ein führendes Unternehmen im Bereich Medizintechnik, sieht als Grundlage für seinen Erfolg die Kultur der kontinuierlichen Verbesserung im Unternehmen. Um sicherzustellen, dass die Mitarbeiter über die Statistikkenntnisse verfügen, die sie benötigen, verlässt sich das Unternehmen auf den Quality Trainer by Minitab, einen E-Learning-Kurs, der Statistik für das Qualitätswesen und die Datenanalyse mit der Minitab Statistical Software vermittelt.
.png)
OneSteel
Als die Menge des sogenannten Walzzunders an Walzdraht aus dem Drahtwalzwerk Laverton von OneSteel Ertrag und Profitabilität der Drahtstraße des Unternehmens beeinträchtigte, setzte das Unternehmen die Six Sigma-Methodik und die Leistungsstärke der Minitab Statistical Software ein, um Lösungen zu finden und den Erfolg nachzuweisen.
.png)
Mosaic Corporation
Erfahren Sie, wie ein Six Sigma-Team der Mosaic Corporation mit seinen umfassenden Erfahrungen bei der Prozessverbesserung und mit leistungsstarken Werkzeugen wie der Minitab Statistical Software die Produktivität um mehr als 50 Prozent steigern konnte, was 12 Millionen US$ pro Jahr entspricht.

DuPont
DuPont Building Innovations konnte die Menge des anfallenden Deponiemülls von 81 Millionen Pfund pro Jahr auf null reduzieren. Das globale Six Sigma-Team, das dieses Ziel umsetzte, nutzte die Minitab Statistical Software, um die riesigen Datenmengen, die während des Projekts erfasst wurden, zu analysieren und auszuwerten.
Halbleiterproduktion
Ein Halbleiterwerk in Thailand setzte die Minitab Statistical Software ein, um den Stromverbrauch genau zu prognostizieren und den Gewinn zu maximieren. Durch Datenanalyse konnte das Werk ein Budget erstellen, in dem der Stromverbrauch an die Produktionsziele angepasst wurde.

Boston Scientific
Bei der jährlichen Bewertung seiner Materialien und Prozesse verwendete der Medizingerätehersteller Boston Scientific die Minitab Statistical Software zum Analysieren von Daten für die Überprüfung des Prozesses, mit dem die Beutel zum Verpacken der Führungsdrähte versiegelt werden. Mit den Werkzeugen in Minitab konnten die Ingenieure souverän mit der Verwendung eines neuen Beutels beginnen, durch den die Verpackung in verschiedenen Unternehmensbereichen optimiert und wesentliche Einsparungen bei den Materialkosten erzielt wurden.

Medtronic
Die Black Belt-Kandidaten bei Medtronic haben unterschiedliche Kenntnisniveaus bei ihrer Vorbildung, was Schulungen erschwert. Um sicherzustellen, dass die Kandidaten in Bezug auf die statistischen Methoden auf dem gleichen Stand sind, und um deren Erfolgspotenzial zu maximieren, entschied sich Medtronic für den Quality Trainer, den E-Learning-Kurs von Minitab für Statistik für die Qualitätsverbesserung.
Stryker
Stryker, ein führendes Unternehmen im Bereich Medizintechnik, sieht als Grundlage für seinen Erfolg die Kultur der kontinuierlichen Verbesserung im Unternehmen. Um sicherzustellen, dass die Mitarbeiter über die Statistikkenntnisse verfügen, die sie benötigen, verlässt sich das Unternehmen auf den Quality Trainer by Minitab, einen E-Learning-Kurs, der Statistik für das Qualitätswesen und die Datenanalyse mit der Minitab Statistical Software vermittelt.

Fresnillo Plc
Fresnillo Plc steigerte den monatlichen Umsatz um über 2 Millionen US-Dollar, indem mit Lean Six Sigma-Methoden und der Minitab Statistical Software der Silbergewinnungsprozess in der Saucito-Mine untersucht wurde.
.png)
Mosaic Corporation
Erfahren Sie, wie ein Six Sigma-Team der Mosaic Corporation mit seinen umfassenden Erfahrungen bei der Prozessverbesserung und mit leistungsstarken Werkzeugen wie der Minitab Statistical Software die Produktivität um mehr als 50 Prozent steigern konnte, was 12 Millionen US$ pro Jahr entspricht.

Newcrest Mining Ltd
Durch die Minitab Statistical Software kann Newcrest Mining in der Cadia Hill-Mine mit jedem LKW eine zusätzliche Ladung Erz pro Tag befördern.

Buckman
Das global operierende Chemieunternehmen Buckman gestaltete seine Abläufe um und schult technische Vertriebsmitarbeiter im Einsatz von Datenanalyse und Minitab, damit sie ihre Kunden bei der Prozessverbesserung unterstützen, den Kunden einen Mehrwert bieten sowie den Umsatz – und den Gewinn – steigern können.

Boston Scientific
Bei der jährlichen Bewertung seiner Materialien und Prozesse verwendete der Medizingerätehersteller Boston Scientific die Minitab Statistical Software zum Analysieren von Daten für die Überprüfung des Prozesses, mit dem die Beutel zum Verpacken der Führungsdrähte versiegelt werden. Mit den Werkzeugen in Minitab konnten die Ingenieure souverän mit der Verwendung eines neuen Beutels beginnen, durch den die Verpackung in verschiedenen Unternehmensbereichen optimiert und wesentliche Einsparungen bei den Materialkosten erzielt wurden.

Cathay General Hospital
Bei einer Auswertung des Angioplastieverfahrens für Herzinfarktpatienten analysierte das Cathay General Hospital in Taipeh (Taiwan) mit der Minitab Statistical Software Daten, um Leben zu retten. Mit den von Minitab bereitgestellten Werkzeugen konnten Medizinexperten neue Behandlungsoptionen einführen, die zu einer Verkürzung des Krankenhausaufenthalts für die Patienten und höheren Einsparungen bei medizinischen Ressourcen führten.

Maxion Wheels
Maxion Wheels, der weltweit größte Hersteller von Autofelgen, benötigte unmittelbare Transparenz in Bezug auf seine Projekte für die kontinuierliche Verbesserung und Operational Excellence. Das Unternehmen entschied sich für Minitab Engage. Diese Lösung bot Workflow-Funktionen, mit denen die Stakeholder den Fortschritt ganz einfach auf der Grundlage von Daten, die sichtbar für die Administratoren sind, nachverfolgen und berichten können. Dadurch konnte das Unternehmen die Transparenz verbessern sowie Zeit und Kosten sparen.

Medtronic
Die Black Belt-Kandidaten bei Medtronic haben unterschiedliche Kenntnisniveaus bei ihrer Vorbildung, was Schulungen erschwert. Um sicherzustellen, dass die Kandidaten in Bezug auf die statistischen Methoden auf dem gleichen Stand sind, und um deren Erfolgspotenzial zu maximieren, entschied sich Medtronic für den Quality Trainer, den E-Learning-Kurs von Minitab für Statistik für die Qualitätsverbesserung.
.png)
DOE bei der Ford Motor Company
In Anbetracht der anstehenden Markteinführung des Ford Fiesta verließ sich die Ford Motor Company auf Minitab, das die erforderlichen Werkzeuge bot, um ein hochwertiges Produkt und einen erfolgreichen Produktstart zu ermöglichen.

Extubationen am Akron Children’s Hospital Center
Der größte Anbieter im Bereich Kindermedizin im Nordosten Ohios analysierte mit Minitab die Daten eines Lean Six Sigma-Projekts. Dies führte zu einer Reduzierung der Anzahl ungeplanter Entfernungen von Beatmungsschläuchen bei Kindern auf der Neugeborenen-Intensivstation und damit zu weniger Komplikationen und einer Verkürzung der Aufenthaltsdauer.

Cummins
Durch den unterschiedlichen Kenntnisstand der Mitarbeiter bei Cummins Inc. in Bezug auf Statistik stellte die Schulung von Six Sigma-Trainees eine Herausforderung dar. Daraufhin probierte das Unternehmen den Quality Trainer by Minitab aus, einen E-Learning-Kurs, in dem Green Belts, Black Belts und andere Qualitätsexperten die Statistikkenntnisse erwerben können, die sie benötigen. Durch die Integration des Quality Trainers in das Schulungsprogramm konnte Cummins mehr Mitarbeiter in Six Sigma-Projekte einbeziehen.

Bobcat
Ein Qualitätsexperte bei Bobcat steigerte mithilfe der Minitab Statistical Software die Geschwindigkeit eines Laserschneidevorgangs bei gleichzeitiger Verbesserung der Teilequalität, was zu möglichen Einsparungen von über 1 Million US$ führte.
Stryker
Stryker, ein führendes Unternehmen im Bereich Medizintechnik, sieht als Grundlage für seinen Erfolg die Kultur der kontinuierlichen Verbesserung im Unternehmen. Um sicherzustellen, dass die Mitarbeiter über die Statistikkenntnisse verfügen, die sie benötigen, verlässt sich das Unternehmen auf den Quality Trainer by Minitab, einen E-Learning-Kurs, der Statistik für das Qualitätswesen und die Datenanalyse mit der Minitab Statistical Software vermittelt.
.png)
OneSteel
Als die Menge des sogenannten Walzzunders an Walzdraht aus dem Drahtwalzwerk Laverton von OneSteel Ertrag und Profitabilität der Drahtstraße des Unternehmens beeinträchtigte, setzte das Unternehmen die Six Sigma-Methodik und die Leistungsstärke der Minitab Statistical Software ein, um Lösungen zu finden und den Erfolg nachzuweisen.

Akron Children’s Hospital
Der größte Gesundheitsdienstleister im Nordosten Ohios setzt Qualitätsverfahren aus der Industrie ein, um die Wartezeiten der Patienten zu verkürzen und eine Vielzahl weiterer Verbesserungen einzuführen. Zum Analysieren der Daten und zum Interpretieren der Ergebnisse verlassen sie sich auf die Minitab Statistical Software.
.png)
Mosaic Corporation
Erfahren Sie, wie ein Six Sigma-Team der Mosaic Corporation mit seinen umfassenden Erfahrungen bei der Prozessverbesserung und mit leistungsstarken Werkzeugen wie der Minitab Statistical Software die Produktivität um mehr als 50 Prozent steigern konnte, was 12 Millionen US$ pro Jahr entspricht.

Newcrest Mining Ltd
Durch die Minitab Statistical Software kann Newcrest Mining in der Cadia Hill-Mine mit jedem LKW eine zusätzliche Ladung Erz pro Tag befördern.

DuPont
DuPont Building Innovations konnte die Menge des anfallenden Deponiemülls von 81 Millionen Pfund pro Jahr auf null reduzieren. Das globale Six Sigma-Team, das dieses Ziel umsetzte, nutzte die Minitab Statistical Software, um die riesigen Datenmengen, die während des Projekts erfasst wurden, zu analysieren und auszuwerten.

RightSource
Als die Apotheke RightSource ein neues Rezeptverwaltungssystem einführte, sank die Produktivität, und Bestellungen fielen in den Rückstand. Durch Umsetzung eines Lean Six Sigma-Projekts mit Minitab konnte das Unternehmen den Umlaufbestand um 40 % reduzieren und bei jedem Arbeitsschritt Geld sparen.

Buckman
Das global operierende Chemieunternehmen Buckman gestaltete seine Abläufe um und schult technische Vertriebsmitarbeiter im Einsatz von Datenanalyse und Minitab, damit sie ihre Kunden bei der Prozessverbesserung unterstützen, den Kunden einen Mehrwert bieten sowie den Umsatz – und den Gewinn – steigern können.

Cathay General Hospital
Bei einer Auswertung des Angioplastieverfahrens für Herzinfarktpatienten analysierte das Cathay General Hospital in Taipeh (Taiwan) mit der Minitab Statistical Software Daten, um Leben zu retten. Mit den von Minitab bereitgestellten Werkzeugen konnten Medizinexperten neue Behandlungsoptionen einführen, die zu einer Verkürzung des Krankenhausaufenthalts für die Patienten und höheren Einsparungen bei medizinischen Ressourcen führten.

Grupo Mutual
Ein Projektteam bei der Grupo Mutual, eines der führenden Finanzinstitute Costa Ricas, wollte den Cashflow zwischen 55 ihrer Bankfilialen verbessern. Mit Lean Six Sigma-Methoden und der Minitab Statistical Software konnte das Team die Erträge um 1,1 Millionen $ steigern.

Edward Jones
In Anbetracht des derzeitigen Wachstums des Finanzdienstleisters und seiner Expansionspläne wollte Edward Jones sicherstellen, dass der erstklassige Kundendienst auch künftig die Erwartungen der Kunden übertrifft. Ausgerüstet mit Lean Six Sigma-Strategien und den Statistikwerkzeugen in der Minitab Statistical Software begann das Prozessverbesserungsteam bei Edward Jones zu untersuchen, wie das Unternehmen bei ständig steigenden Anforderungen weiterhin die hohen Standards beim Kundendienst einhalten konnte.

SOCOMEC
Der Stromnetzspezialist Socomec setzte die Minitab Statistical Software und Lean Six Sigma-Methoden ein, um Vertriebsprozesse zu messen und zu verbessern.

Personalwesen
Im Rahmen einer Untersuchung der hohen Personalabgangsrate führte die Personalabteilung eines großen Herstellers von Maschinenteilen für die Luft- und Raumfahrt ein Lean Six Sigma-Projekt durch und nutzte hierbei die Statistikwerkzeuge der Minitab Statistical Software für die Datenanalyse.

Akron Children’s Hospital
Der größte Gesundheitsdienstleister im Nordosten Ohios setzt Qualitätsverfahren aus der Industrie ein, um die Wartezeiten der Patienten zu verkürzen und eine Vielzahl weiterer Verbesserungen einzuführen. Zum Analysieren der Daten und zum Interpretieren der Ergebnisse verlassen sie sich auf die Minitab Statistical Software.



